Helping to reduce risk (and save time) with ready-to-administer syringes
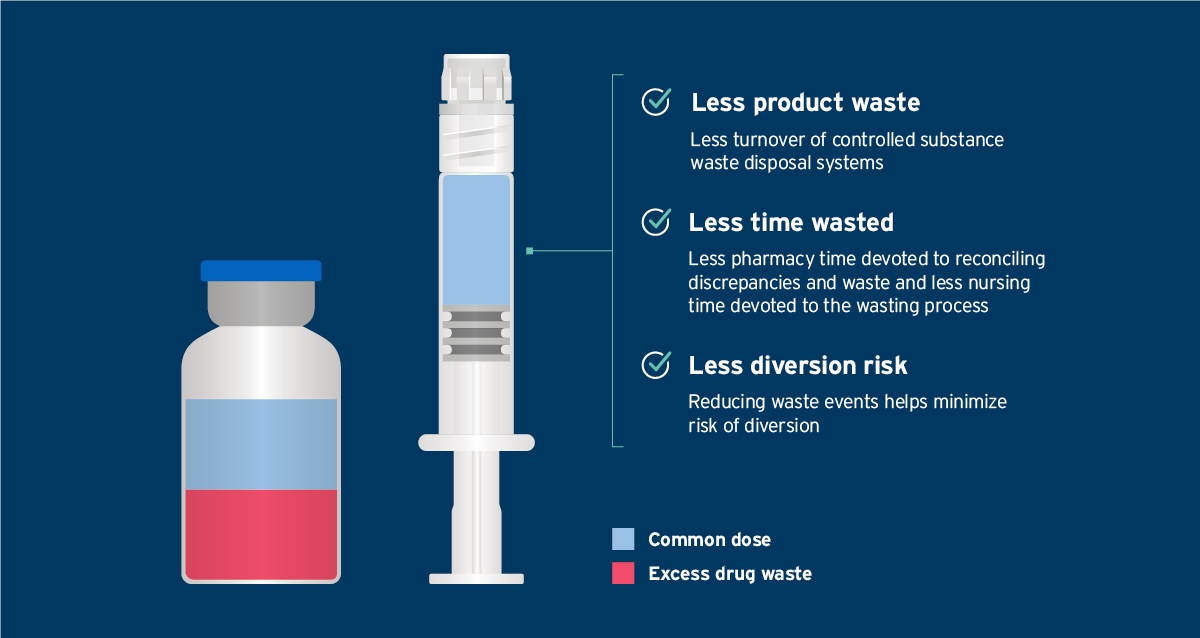
Photo: Fresenius Kabi
Administering medication in an acute setting can come with significant waste. In a recent study, researchers discovered that the cost associated with wasting morphine, fentanyl and hydromorphone was approximately $2.40 per dose. 1 While that number may seem small at first glance, when one considers every medication administration, every day, as well as the required clinician time to manage those doses, these preventable expenses add up to tens of thousands of dollars of waste each year. They also significantly increase opportunities for medication diversion.1 Those are just a few of the reasons why Baptist Health, a full-spectrum health system in Kentucky and surrounding states, opted to move to manufacturer-prepared Simplist® MicroVault pre-filled syringes, said Nilesh Desai, Chief Pharmacy Officer.
“Waste management is a huge challenge. Our goal is to provide the right dose of the medication to the right patient at the right time – in a single form,” he explained. “Having ready-to-administer syringes, in exact doses, reduces that unnecessary waste and the potential for diversion.”
Brandon McLain, PharmD, Director of Pharmacy Operations at Baptist Health, agreed, adding that ready-to-administer syringes can help improve patient safety. A recent study* found that ready-to-administer syringe products were associated with an error rate four times lower than IV push traditional practice methods.2
*Simplist was the only RTA delivery system used in the study.
*Study limitations include only a select number of sites (3) and steps observed.
"Consider emergency situations,” he noted. “If your clinicians are working with a vial during a high-stress event, they have to take the time to make sure they have the right dose. We know those manual manipulations can lead to errors and safety issues. Having something pre-filled and ready to go lessens the probability of a medication error occurring.”
The use of ready-to-administer syringes also helps clinicians save time and reduce frustration, particularly when used in tandem with automated, single-dose dispensing systems. Nurses especially appreciate the ease and efficiency of this kind of setup, according to Desai. “Nurses are pulled in so many directions – when they are asked to help a patient or assist a doctor, they may get distracted. Those distractions, unfortunately, can lead to errors,” he explained.
For example, this setup reduces the need for manual countbacks, an extremely frustrating and time-consuming task, McLain pointed out. “The typical workflow with dispensing a controlled substance is that the nurse has to count the medication, put in a number, take the medication and go,” he said. “There’s added time involved with counting correctly, as well as a possibility for diversion because that nurse has access to all the stock loaded in that pocket and not just what’s required for their patient. With ready-to-administer syringes, the pharmacy loads the drawers with these cassettes. The nurse then clicks that they need one syringe for a patient, the syringe drops into the drawer, the nurse grabs it and goes. It means there’s one less thing that the nurses have to do.”
Given the benefits of ready-to-administer syringes, Desai said that he hopes to see manufacturers offer additional pre-filled medications in a more diverse range of doses in the future.
“This kind of system shines a light on areas that are still a blind spot for many health systems across the country,” he said. “When you put all the benefits together, you see that ready-to-administer syringes make sense. They are significantly beneficial to controlled substance monitoring and control.”
References
- Hertig, J., Jarrell, K., Arora, P. et al. A continuous observation workflow time study to assess intravenous push waste. Hosp Pharm.56(5):584-591. doi: 10.1177/0018578720931754.
- Hertig, J., Degnan, D., Scott, C., et al. March 2018. A comparison of error rates between intravenous push methods: a prospective, multisite, observational study. Journal of Patient Safety 14(1):60-65. doi: 1097/PTS.0000000000000419.
3671-FNCI-08-01/23



7993.jpg)